An inflammatoryprocess causes bone resorption that may lead to subsequent loosening of the hip implants and even fractures in the bone around the implants. This is the loss of bone caused by the body's reaction to polyethylene wear debris, fine bits of plastic that come off the cup liner over time. Many long-term problems with hip replacements are the result of osteolysis. Post-operative femoral fractures are graded by the Vancouver classification. Fracture īones with internal fixation devices in situ are at risk of periprosthetic fractures at the end of the implant, an area of relative mechanical stress. Use of alcohol by patients during this early period is also associated with an increased rate of dislocation. Patients can decrease the risk further by keeping the leg out of certain positions during the first few months after surgery. Doing the surgery from an anterior approach seems to lower dislocation rates when small diameter heads are used, but the benefit has not been shown when compared to modern posterior incisions with the use of larger diameter heads. Surgeons who perform more of the operations each year tend to have fewer patients dislocate. The chance of this is diminished if less tissue is cut, if the tissue cut is repaired and if large diameter head balls are used. 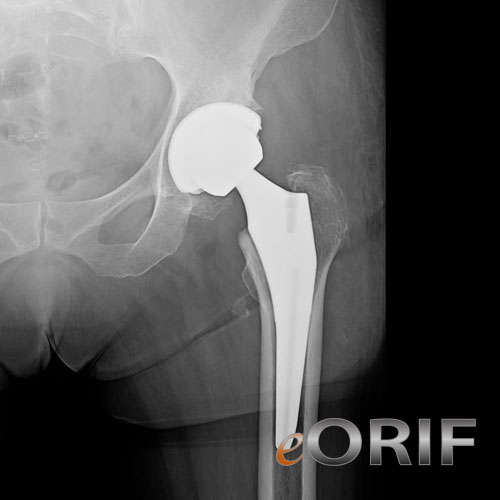
During this period, the hip ball can come out of the socket. It takes eight to twelve weeks for the soft tissues injured or cut during surgery to heal. At surgery the femoral head is taken out of the socket, hip implants are placed and the hip put back into proper position. Dislocation ĭislocation is the most common complication of hip replacement surgery. However, this kind of screening should only be done when indicated because to perform it routinely would be unnecessary health care. Some physicians and patients may consider having lower limbs venous ultrasonography to screen for deep vein thrombosis after hip replacement. Standard treatment with anticoagulants is for 7–10 days however treatment for more than 21 days may be superior. Venous thrombosis such as deep vein thrombosis and pulmonary embolism are relatively common following hip replacement surgery. They can include dislocation, loosening, impingement, infection, osteolysis, metal sensitivity, nerve palsy, pain and death. Risks and complications in hip replacement are similar to those associated with all joint replacements. Hip prosthesis displaying aseptic loosening (arrows) Hip replacement is usually considered only after other therapies, such as physical therapy and pain medications, have failed. 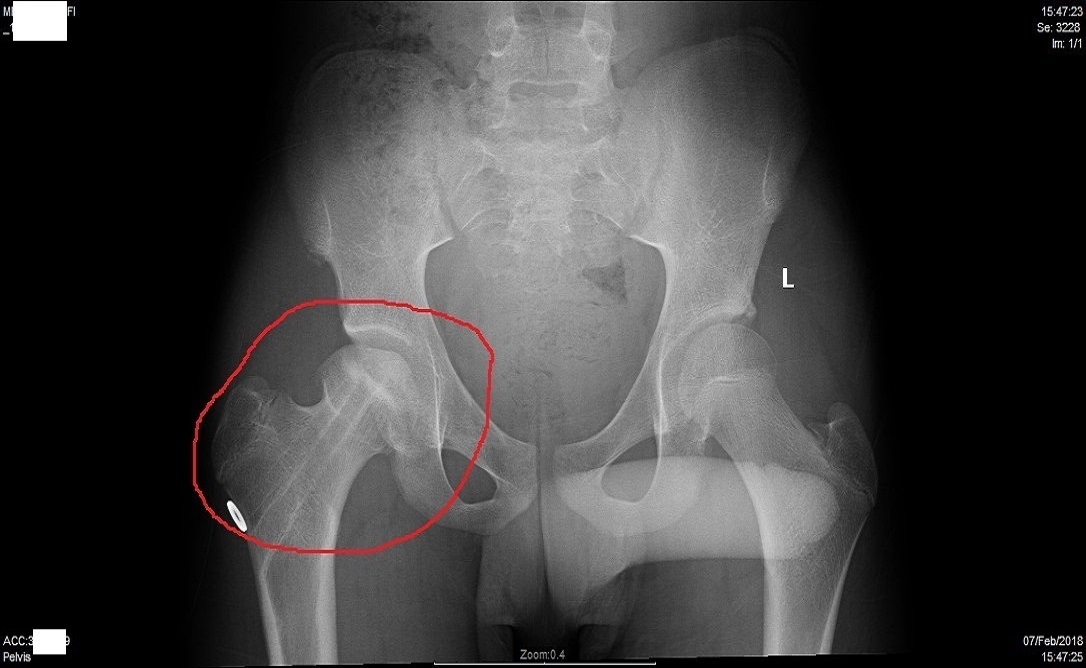
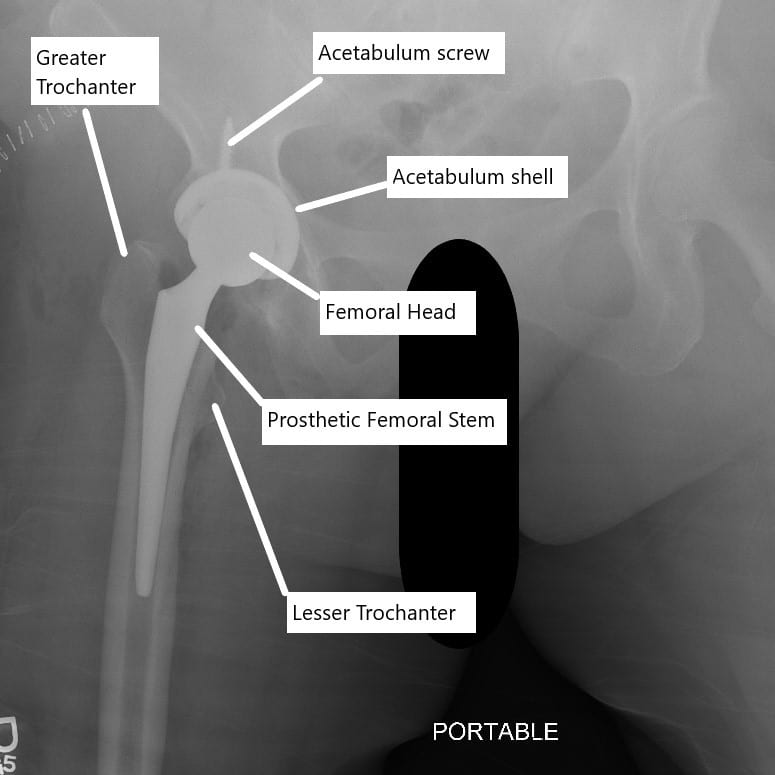
The aims of the procedure are pain relief and improvement in hip function. Other indications include rheumatoid arthritis, avascular necrosis, traumatic arthritis, protrusio acetabuli, certain hip fractures, benign and malignant bone tumors, arthritis associated with Paget's disease, ankylosing spondylitis and juvenile rheumatoid arthritis. Total hip replacement is most commonly used to treat joint failure caused by osteoarthritis. Hip replacement is currently the most common orthopaedic operation, though patient satisfaction short- and long-term varies widely. A total hip replacement (total hip arthroplasty) consists of replacing both the acetabulum and the femoral head while hemiarthroplasty generally only replaces the femoral head. Such joint replacement orthopaedic surgery is generally conducted to relieve arthritis pain or in some hip fractures. Hip replacement surgery can be performed as a total replacement or a hemi (half) replacement. Hip replacement is a surgical procedure in which the hip joint is replaced by a prosthetic implant. Total hip replacement.An X-ray showing a right hip (left of image) has been replaced, with the ball of this ball-and-socket joint replaced by a metal head that is set in the femur and the socket replaced by a white plastic cup (clear in this X-ray). The effect of patient age at intervention on risk of implant revision after total replacement of the hip or knee: a population-based cohort study. Lespasio MJ, Piuzzi NS, Husni ME, Muschler GF, Guarino A, Mont MA. Prognostic factors for progression of osteoarthritis of the hip: a systematic review. Teirlinck CH, Dorleijn DMJ, Bos PK, Rijkels-Otters JB, Bierma-Zeinstra SMA, Luijesterburg PAJ. Glucosamine and chondroitin sulfate: what has been learned since the Glucosamine/Chondroitin Arthritis Intervention Trial. TGF-β signaling and the development of osteoarthritis.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |

 RSS Feed
RSS Feed
